Commentary
Article
Herpes Zoster as an Early Indicator of HIV: Clinical Insights
Author(s):
The risk of developing HZ in this population is 10 to 30 times higher than in the general population.
Herpes zoster (HZ), commonly known as shingles, is a frequently occurring opportunistic infection in individuals living with HIV. Without antiretroviral therapy (ART), the risk of developing HZ in this population is 10 to 30 times higher than in the general population. Even with ART, the risk remains about 3 times higher, likely due to more significant immunosuppression.
Image credit: snesivan | stock.adobe.com
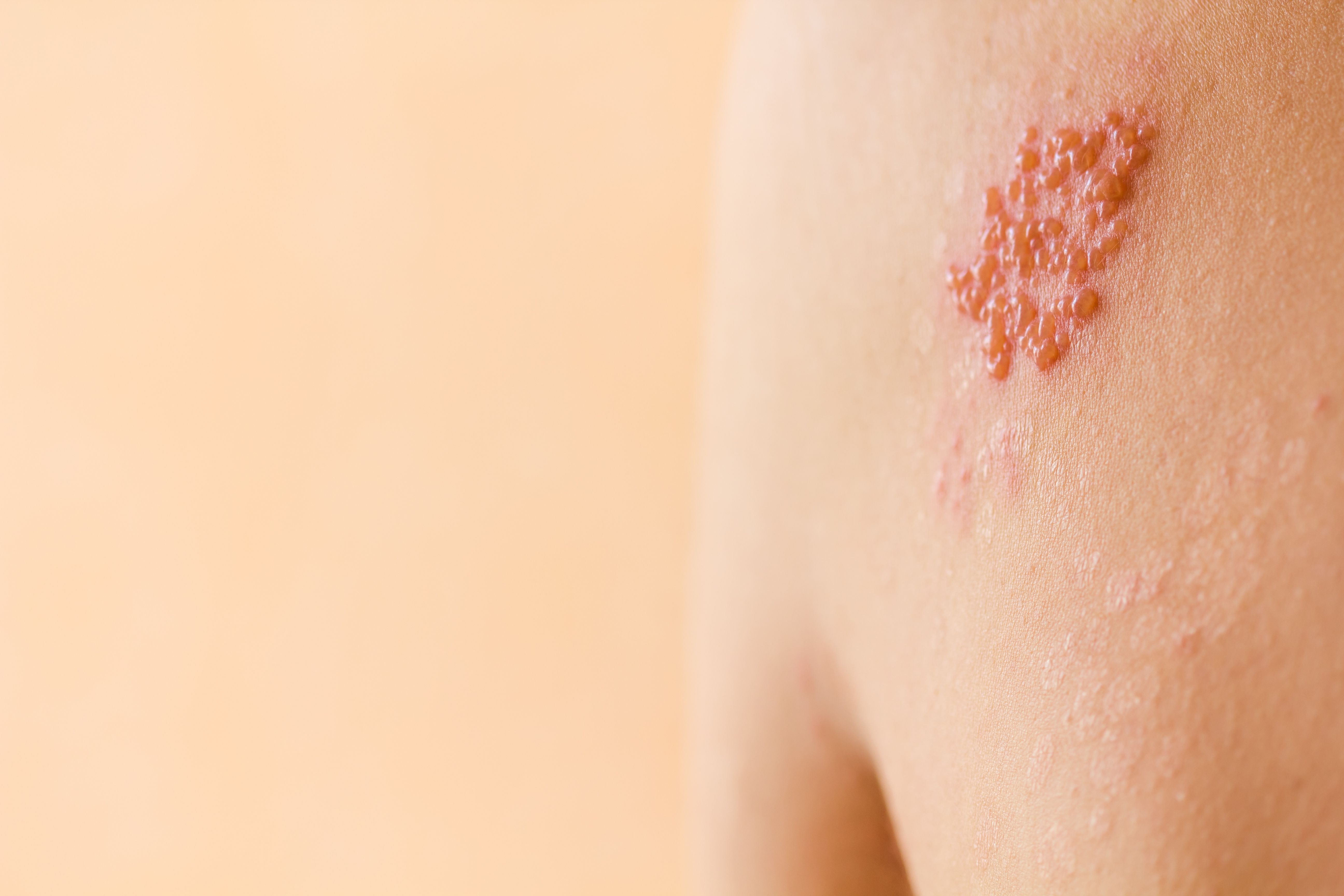
Results of a retrospective study published in the International Journal of STD & AIDS in February 2025 highlights the critical role of herpes zoster infection as an early indicator of undiagnosed HIV. Researchers studied 45 cases of individuals with HIV diagnosed with herpes zoster from January 2015 to September 2024. The participants were predominantly male with a mean age of approximately 36 years.
Among the patients, 21 were actively treated with ART and 6 developed HZ shortly after starting therapy. This suggests a link to immune reconstitution inflammatory syndrome (IRIS), a condition that can activate an inflammatory response against latent infections. Most notably, in 12 patients, the manifestation of herpes zoster served as the initial indicator of HIV diagnosis.
Research continuously shows that a low CD4 count is a strong predictor of HZ, though risk remains significant at any level. This strongly suggests that patients who present with HZ, especially younger individuals with no known underlying immunosuppressive conditions, should be tested for HIV.
Early HIV detection allows for timely initiation of ART. This is essential for reducing viral transmission, reducing the occurrence of opportunistic infections, and slowing disease progression. Additionally, prompt treatment of HZ is crucial to reduce complications and optimize patient outcomes. Studies show initiating antiviral therapy with treatments such as acyclovir (Sitavig; BioAlliance Pharma) can reduce the risk of postherpetic neuralgia by 50%. Furthermore, the shingles vaccine may be a preventive measure in appropriate patients to reduce the risk of HZ and its complications.
Pharmacists are crucial for early detection, education, and treatment optimization in patients with HZ and suspected HIV. Health care professionals as a whole should prioritize HIV screening, especially in young patients presenting with HZ with no other risk factors. Providers should also be vigilant in educating and monitoring for IRIS-related HZ within the first 6 months of initiating ART. By integrating these management strategies, clinicians can enhance and optimize health outcomes in this at-risk population.
Reference
Guechchati M, Sougha M, Rabhi S, et al. Shingles in HIV: outcome and discovery. Int J STD AIDS. 2025;9564624251324975. doi:10.1177.09564624251324975
Newsletter
Stay informed on drug updates, treatment guidelines, and pharmacy practice trends—subscribe to Pharmacy Times for weekly clinical insights.





